Finding blood in your stool can be alarming and may indicate a range of potential health issues. While it’s not uncommon to experience this symptom occasionally, especially if you have hemorrhoids, persistent or unexplained blood in the stool should be evaluated by a healthcare professional. Understanding the possible causes and when to seek medical advice is crucial for addressing this issue effectively.
Common Causes of Blood in Stool
- Hemorrhoids:
- Swollen veins in the lower rectum and anus can rupture and cause bright red blood in the stool. This is often accompanied by itching or discomfort.
- Anal Fissures:
- Small tears in the lining of the anus can occur due to passing hard stools. These tears can cause pain and bright red bleeding during bowel movements.
- Diverticular Disease:
- Diverticula are small pouches that can form in the walls of the colon. If these become inflamed or infected, they can lead to bleeding.
- Inflammatory Bowel Disease (IBD):
- Conditions such as Crohn’s disease and ulcerative colitis can cause inflammation and ulcers in the digestive tract, leading to blood in the stool.
- Gastrointestinal Infections:
- Bacterial, viral, or parasitic infections can cause inflammation and bleeding in the intestines, resulting in blood in the stool.
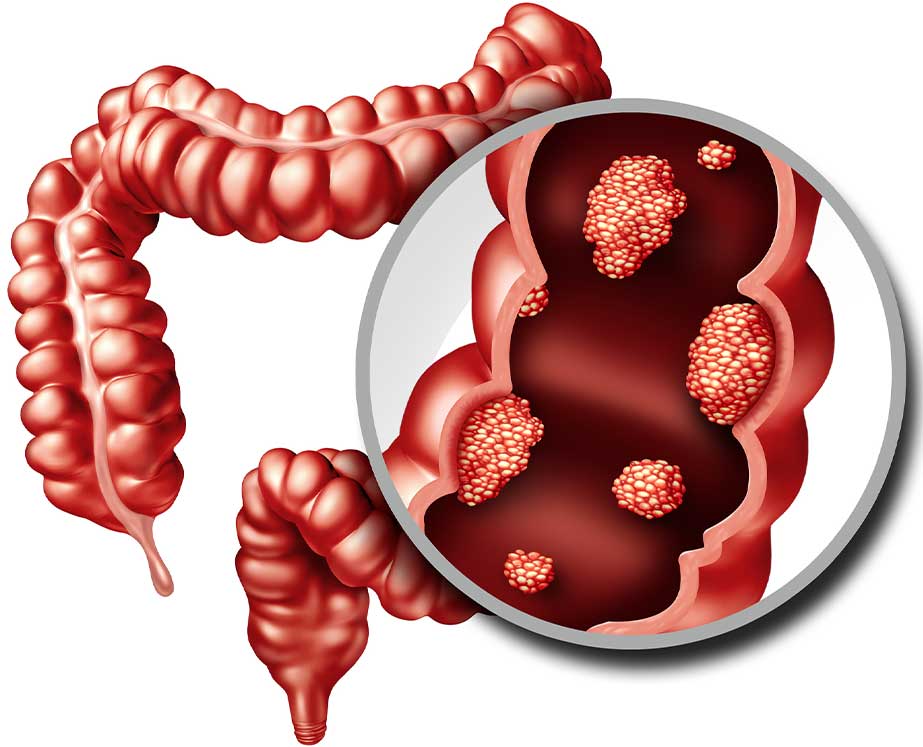
- Polyps or Cancer:
- Colorectal polyps are growths on the inner lining of the colon or rectum and can bleed. Over time, some polyps can develop into cancer, which may cause bleeding.
- Peptic Ulcers:
- Ulcers in the stomach or upper part of the small intestine can bleed, leading to dark, tarry stools.
When to Seek Medical Help
If you notice blood in your stool, especially if it occurs frequently or is accompanied by other symptoms such as abdominal pain, weight loss, or changes in bowel habits, it is essential to consult a healthcare professional. Early evaluation and diagnosis are crucial for effective treatment and management.
Steps for Managing Blood in Stool
- Medical Evaluation:
- Schedule an appointment with your healthcare provider to discuss symptoms and undergo necessary diagnostic tests, such as a colonoscopy, to determine the cause of bleeding.
- Dietary Adjustments:
- Increase fiber intake to soften stools and reduce straining. Focus on a balanced diet rich in fruits, vegetables, and whole grains to promote digestive health.
- Hydration:
- Drink plenty of fluids to help maintain regular bowel movements and prevent constipation, which can exacerbate bleeding.
- Over-the-Counter Remedies:
- Consider using stool softeners or fiber supplements to ease bowel movements if recommended by your healthcare provider.
- Lifestyle Changes:
- Incorporate regular exercise into your routine to improve bowel function and reduce stress.
By understanding the potential causes of blood in the stool and taking proactive steps, you can manage symptoms and improve your digestive health. Remember, persistent or unexplained bleeding should not be ignored, and timely medical consultation is key to preventing complications.
Blood